Testing Americans’ views on testing
Volume 13, Issue 2 | January 15, 2026
IN THIS ISSUE
Two new biomarkers for subtyping MS
Two more diagnostic uses for your cell phone
Today’s patients expect more authority over testing
A pulse oximeter that looks beneath the skin’s pigment layer
Infectious disease update: Flu and measles
Two new biomarkers for subtyping MS
The initial diagnosis of multiple sclerosis has long been challenging. It’s considered a “diagnosis of exclusion” — only after you’ve ruled out all other possible causes (including lyme, lupus, vasculitis, and other conditions), can you say your patient has MS. Today, MRI of the brain and spinal cord plus analysis of cerebrospinal fluid can help, but it is not a perfect science.
Adding to the complexity is that MS is not one condition, but multiple. Its subtypes include clinically isolated syndrome (only sometimes indicating early MS), relapsing / remitting MS (a myelination/white-matter disorder representing 80-plus percent of MS cases, for which current drugs can be effective) to primary progressive MS (a later inflammatory stage of the disease, for which there are currently no effective treatments).
Two new biomarker tests have the potential to help with this staging / subtyping challenge.
One, which is closer to use in the clinic, resulted from AI analysis of patterns between blood biomarkers and brain images of 634 MS patients. During the course of this work, two new subtypes of relapsing / remitting MS became apparent: One with high levels of neurofilament light chain (Nfl) in the blood, which was likely to progress quickly, and one with lower Nfl levels, which didn’t.
The other biomarker is at an early stage of research. That work found that the ratio of two proteins (CXCL13:BAFF) in cerebrospinal fluid was an early signal of the gray matter destruction typically only detected much later in progressive MS.
COMMENTARY: Reliable subtyping of any disease, MS included, is critical to true personalized medicine. Not only does it allow clinicians to set patients’ expectations more effectively, it is essential to creating better treatments.
A pulse oximeter that looks beneath the skin’s pigment layer
Pulse oximeters, the tools used to measure how well blood is oxygenated, are notoriously inaccurate for people with darker skin. A new polarization-sensitive sensor could improve things. The sensor uses the orientation of the light it receives to filter out signals from the superficial layers of the skin, where pigment is present. That allows it to capture signals from deeper tissue.
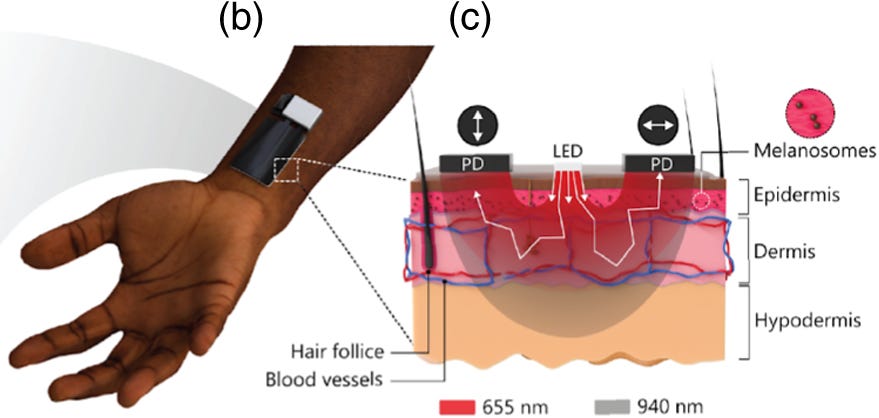
Until last week, available evidence indicated that pulse oximeters tend to overestimate how well-oxygenated blood is in people with more skin pigment. That’s a potentially life-threatening problem, because it could cause people who need supplemental oxygen to be missed.
However, that conclusion came from retrospective studies. As STAT News explained it, “the data used was not collected explicitly to study pulse oximeters.” So the FDA funded a prospective study to clear the issue up.
It did the opposite. A preprint of the study appeared last Friday. It found that pulse oximeters underestimated blood oxygenation levels. Part of the issue, the researchers note, is that most of the patients in the study were so well oxygenated that there wasn’t much room for the devices to overestimate their oxygen levels at all. (The average blood oxygenation level was 98%.) People also weren’t included in the study if their oxygenation levels weren’t stable.
Regardless, the study still found that pulse oximeters didn’t work as well as they should — their overall sensitivity for detecting low blood oxygen levels was 72%.
COMMENTARY: A better pulse/ox solution is clearly still needed. And one that bypasses the pigment layer of the skin altogether seems like a very good idea.
Two more diagnostic uses for your cell phone
One of the most common wearable devices is probably sitting in your pocket right now. We came across two new uses for it recently — and they’re both likely to have better health effects than doomscrolling. (Okay, we realize that’s a low bar. But still.)
A relatively small study of patients with rheumatoid arthritis (292 patients) found that their cell phones were able to pick up subtle changes in their behavior that indicated an impending disease flare-up: Slower reaction times and fewer texts. Usually patients don’t notice disease flare-ups happening until the symptoms are pretty bad. Earlier detection would allow for earlier bump-ups in treatment, thereby heading off more severe symptoms.
Another small study (60 patients) showed that smartphones could be effectively used to diagnose sleep apnea in people who’ve had a stroke. (About half of stroke patients have the condition.) The diagnosis relied partly on tools the phones already had — audio for recording sound and accelerometry for tracking movement — plus a wireless pulse oximeter to measure blood oxygen levels.
Today’s patients expect greater authority over testing decisions
Patient empowerment has become a strong force in diagnostic testing, especially among the wealthy worried well. Just how strong it is has been demonstrated by a national survey commissioned by Siemens Healthineers and conducted by YouGov.
Some results of note:
Diagnostic testing is viewed as both important and valuable. 98% believe test results to be insightful, 96% trust those results to be accurate, and 94% are more willing to accept physician advice when supported by test results.
The pandemic left a legacy of increased confidence in self-testing. 71% have performed a self-test in the past two years — 49% for a specific illness, 22% out of general curiosity.
Patient-initiated testing was most common among Millennials (those born 1981 – 96). 94% of them had administered a self-test, in contrast to 45% of those born before 1945.
Patient empowerment is growing. 93% expect their doctor to agree to any test they request, and 78% believe they can interpret the results without professional help.
However, trust in physicians remains strong. 95% trust their physicians to order the right tests, and 87% would not take a test if their physician advised against it.
Interest in predictive testing is also strong, with 89% interested in risk prediction.
COMMENTARY: Diagnostic testing is undergoing a revolution. As we have described many times - new, less-invasive tests, for a broader menu of available conditions, available without physician orders, promise to dramatically increase the number of tests taken.
However, the US primary-care delivery model is already under stress. As patient-initiated testing grows, care delivery and follow-up face even more challenges — a problem covered in a recent STAT News article, the first of a series on direct-to-consumer testing.
Another concern is that while interest in predictive testing implies a strong endorsement of asymptomatic / presymptomatic screening (e.g., multi-cancer early detection tests, whole-body MRIs, etc.), it also implies a lack of knowledge and / or concern about the full extent of false positives.
Nevertheless, this report is a strong endorsement of the value of diagnostic testing. It should be a clear signal to the entire health-care system that patients, aka customers, value diagnostic testing and want it to play a central role in their personal health care.
We’re interrupting this section’s usual monthly cadence to bring you some significant news that came out this week.
Influenza
Your Local Epidemiologist reported that the rate of influenza-like illness “is the highest it has been since 1997-98 (nearly 30 years), and the highest on record since the CDC started tracking.” And we’re not at the peak of the season yet.
Measles
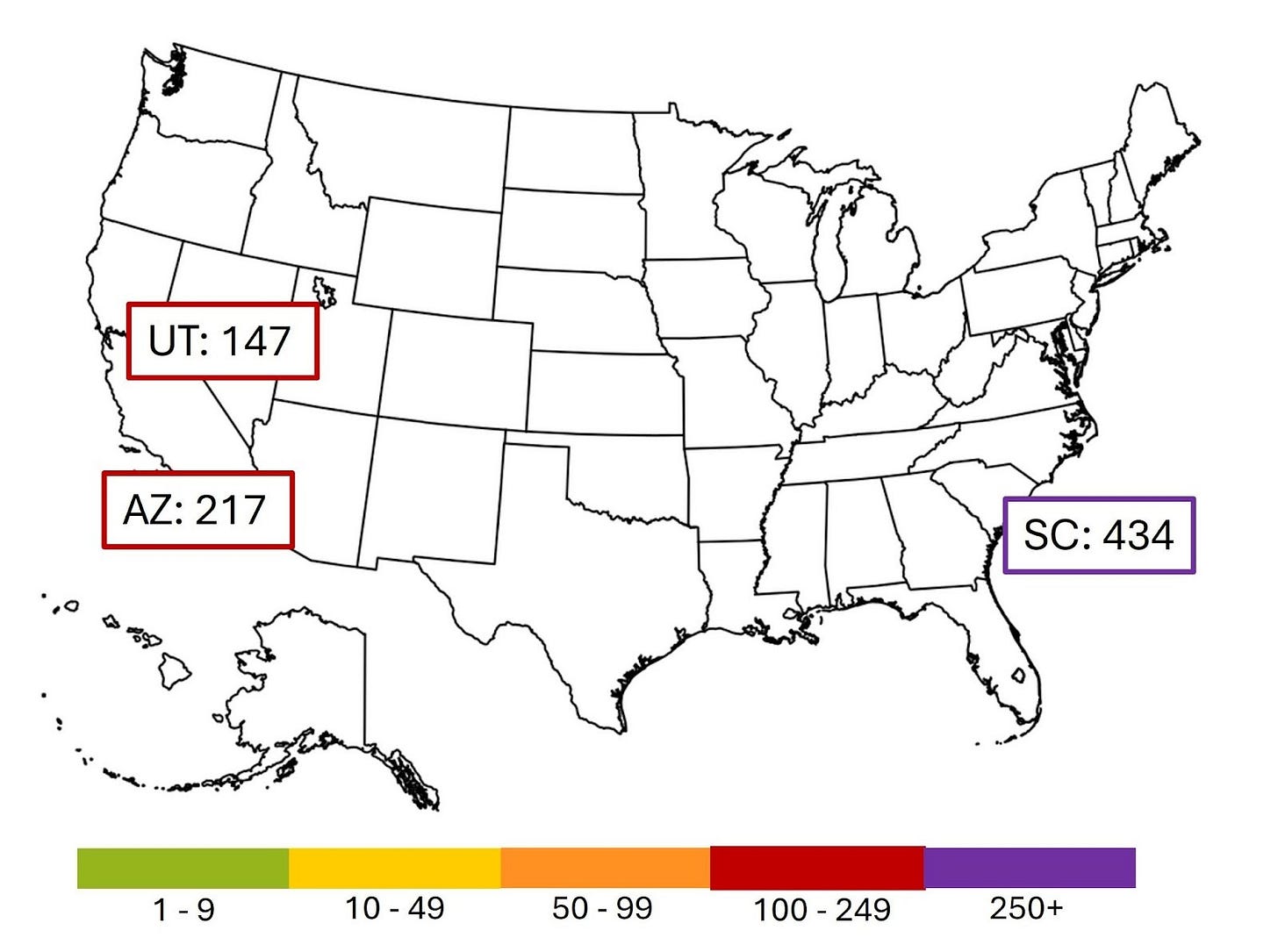
Over the last week, the measles outbreak in South Carolina grew by 124 cases, to 434. “The last time the U.S. saw more than 100 cases in a single week was the worst parts of the West Texas outbreak last spring,” STAT News reports. Related measles cases also appeared in North Carolina and Ohio, in families who had traveled to the area in South Carolina affected by the outbreak. The current larger outbreaks in the US are shown below: Arizona / Utah, South Carolina.








Thank you, thank you for continuing to provide such valuable information. The work you do is SO important and appreciated!
Amy in Boston
Nice article - thank you!