ALSO IN THIS ISSUE
Keeping an eye on Omicron’s brood of descendants
Will Europe be a bellwether for the US again this fall/winter?
New and Noteworthy
Watching New Sub-Variants - and Europe’s Fall Surge
We’ve entered the fourth quarter of The Year of Omicron. The folks who follow variants are currently tracking . . . wait for it . . . 23 sub-lineages of the Big O.
In the US, the current top three sub-variants are:
BA.5: 19.2%
BA.4.6: 13.6%
BF.7: 4.6%
While BA 4.6 looks ominous (we hear reports that it will evade current vaccines as well as the antibody prophylactic Evusheld), its growth has been very slow - it has grown only 3 points in the last month. Other variants in the mix also have immune escape potential, but as of now they only hold tiny percentages here. It is unclear whether any will “win out” and potentially cause another surge. Fingers crossed that a brand-new variant as different from Omicron as Omicron was from Delta doesn’t rear its ugly head.
All that being said, cases in Europe have notably increased over the last two weeks (Germany - 117% / Italy - 83% / England - 76% / France - 49%). But no single variant is to blame there. Instead, the cause is multifactorial - a soup of new variants, more indoor activities as winter approaches, plus a broad decrease in mitigation behaviors. Is that a preview for the US? Data is not conclusive - we followed Europe into the Omicron surge, but never had as tough of a time with Alpha as they did.
Food for Thought
Focus on Success: Where the Response to COVID Went Right
This week, we look at places where the COVID response worked. As we continue to debate which lessons we should take away from the pandemic experience, these are the places we should be looking at - the models from which our plans should begin.
Testing can Make a Difference - Once People Believe in it
We’ve been banging the “Testing is the best way to find and stop a surge” drum forever. Guess what? Thanks to an article in Politico, we finally found a place that did it: Davis, Calif.
So, what did Davis do? Their program, Healthy Davis Together, managed to get an entire university town invested in the idea of frequent COVID testing as a way to keep outbreaks from happening among its residents.
How did they do it?
UC-Davis put enough testing infrastructure in place to provide free twice-weekly testing for its students, staff, and all town residents. That required buy-in and funding from university administrators, plus collaboration across academic departments from plant science to medicine to engineering.
They had money: An anonymous $40 million donation.
The university ran a major-league PR campaign throughout the town, focused on “getting people to understand the importance of testing.” That campaign brought information about the testing program to people everywhere they were: both at home (mailers, print and digital advertising, door hangers, and Spanish-language radio) and in the community (on billboards, in train stations, on coffee sleeves and takeout napkins, on banners designed by local artists, and in person, in the form of college-student public-health ambassadors). Regular surveys and focus groups kept tabs on the effectiveness of the campaign’s messaging.
The town provided quarantine and isolation support, including housing and salary assistance if needed - thereby removing one of the main reasons why people might not want to test.
The result: An independent evaluation by Mathematica found that between October 2020 and January 2022, the program reduced COVID cases in Davis by 60% compared to what they would have been had the program not been in place.
COMMENTARY: The devil, as always, is in the details, but Davis at least proved that a robust testing program can make a tremendous difference in the public health of a town. And now that they’ve invented that wheel, other places don’t need to reinvent it, at least not completely - the program has helpfully placed how-to information all over their website.
Inequity in Vaccine Access can be Overcome - if it is a Priority
When COVID vaccines first arrived in late 2020, they went exactly where you would expect in a nation with drastic socioeconomic inequities in health-care access: Into the arms of affluent white folks. Birmingham, Alabama, was a case in point, per The Morning Newsletter from the New York Times just over a week ago: “The Black neighborhoods didn’t have vaccines, and the white areas did.” Yet by the end of November 2021, CDC data indicated that the nationwide racial gaps in vaccination coverage had essentially disappeared.
So what changed? Presidential priorities and communication. Rather than simply distributing vaccines to the states and stepping back, the Biden administration made vaccines and vaccination equity a focus. Among multiple efforts in this area, it ensured that community health clinics received vaccines and worked with local organizations (from Healthy Truckers to 100 Black Men to local county fairs) to provide vaccination in places where people in the community wanted to go.
COMMENTARY: Just like money, health access doesn’t simply trickle down. If you want to get vaccines to people who need them, you have to make sure that those vaccines go all the way to where they’re needed, and into venues where people feel comfortable accessing them. And you won’t know what those places are unless you ask the folks who live there.
You can Protect Your (Small) Country - if People Understand the Guidelines and are Willing to Follow Them
Several thoughtful pieces have been published in the past few weeks comparing Japan's successful COVID response to the US’s relative failure: an Economist feature, an Eric Topol Ground Truths blog, and a pandem-ic.com feature, to name just a few.
What’s behind Japan’s success?
Much higher masking adoption than the US (it has long been considered rude in Japan to blow your nose in public or to sneeze in public without a mask on)
Consistent, clear, and evidence-based public health communication about avoiding “the three Cs”: closed spaces, crowded places, and close-contact settings
High vaccination rates for all but the most traditional/oldest (despite significant vaccine reluctance - Japan’s is rooted in a 30- year-old narrative about unproven MMR side effects)
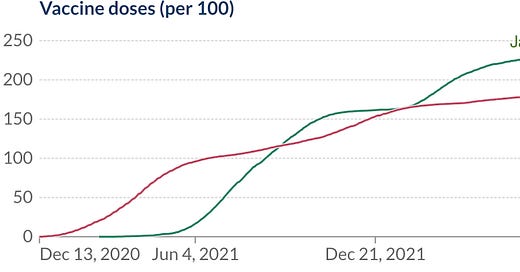
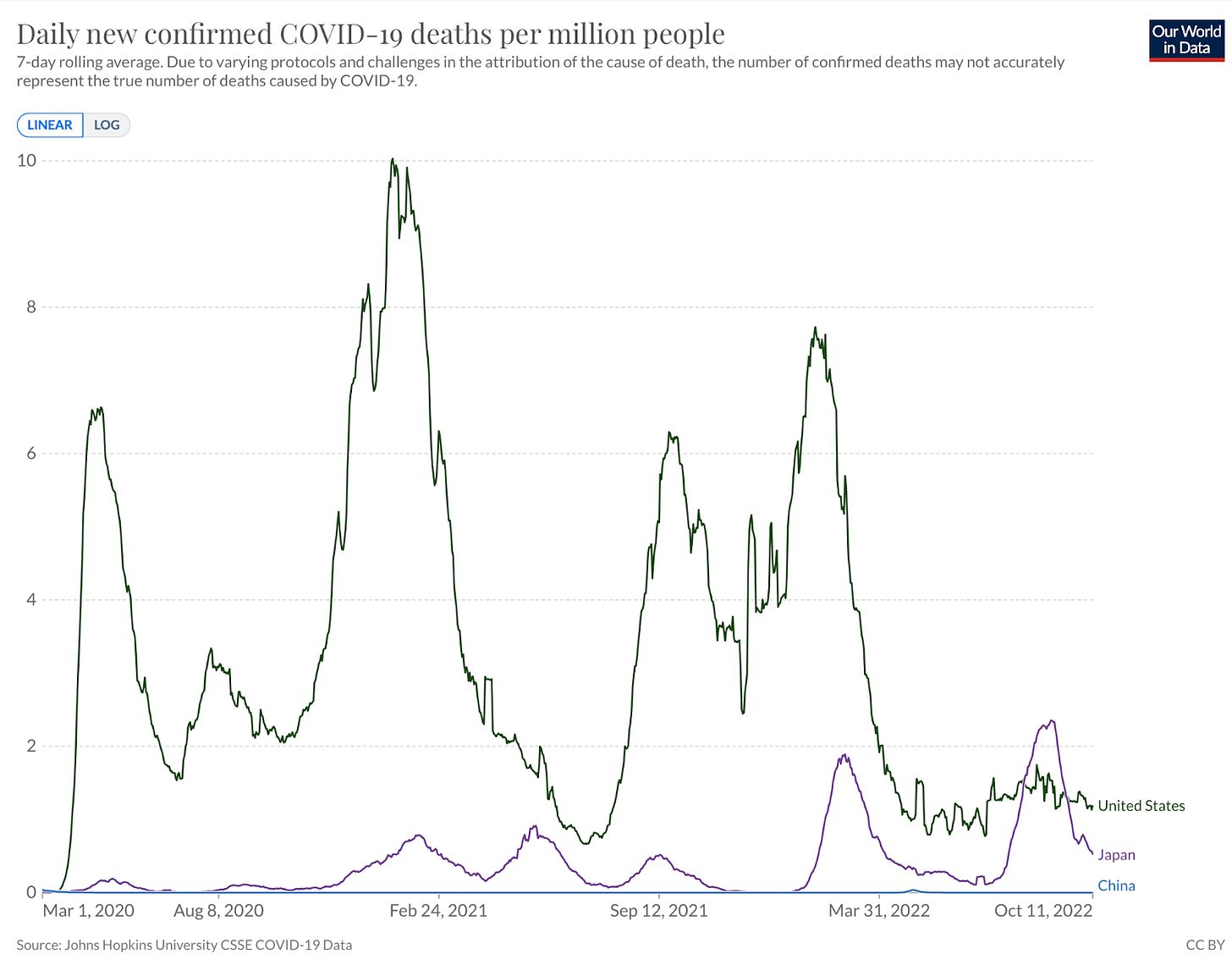
You can see the results below (from Oxford University’s Our World in Data). Granted, Japan is much smaller and more homogenous than the US, but the differences here could hardly be more stark - in both vaccine doses per 100 people and most importantly, the consequent deaths per million people.
For the Lucky Few, the Right Genes are all you Need
Okay, so this one isn’t a lesson learned, but we’ll throw it in here because we’re science nerds, and it’s cool. You know how lots of people who get infected with COVID never have symptoms - as in no symptoms at all? Turns out that about 10% or so of the overall population has a genetic mutation that helps them clear the virus so fast, they don’t have time to get sick. We should all be so lucky.
Quick Hits
The FDA has now Granted Two EUAs for Commercial Monkeypox Tests
The first went to Quest Diagnostics; Abbott received authorization for theirs this week. Of note - these are both PCR, lab-based tests, and they’re both proprietary. The CDC assay was shared with the five top labs in the country (Aegis, LabCorp, Mayo, Quest, Sonic) back in June.
Uganda is in the Midst of a Small but Worrisome Ebola Outbreak
The numbers so far may seem relatively low (44 confirmed cases with 10 deaths), but Ebola is far more contagious than COVID and has a presymptomatic stage (although it is believed that only symptomatic people can spread disease). As a result, testing is now required for all travelers coming to the US from Uganda.
New Data Continues to Confirm that Home Antigen Tests Still Work for Omicron.
In fact, a secondary analysis of a late 2021/early 2022 found that these tests were slightly more effective at detecting Omicron (BA.1.1.529) than Delta (B.1.617.2), although the difference was not statistically significant.